My aunt was discharged from a London hospital in November 2023 after a cardiac event. Seventy-two hours after leaving the ward, a wearable patch on her chest detected an arrhythmia. It didn’t beep. It didn’t alert her. It silently transmitted the data to her cardiologist’s dashboard, who called her before she’d even noticed anything was wrong. This is how future healthcare technology is elevating at-home care.
No ambulance. No A&E queue. No hospital readmission.
That moment a quiet, invisible, data-driven intervention that happened inside her own living room is what the future of at-home healthcare actually looks like. Not science fiction. Not five years away. Happening right now, in houses and flats across the USA and UK, to people who thought “home care” still meant a district nurse coming by on Thursdays.
The technology driving this shift is moving faster than most patients, carers, and even healthcare providers realize. And with Google’s March 2025 core algorithm update fundamentally reshaping how health information ranks online, understanding how to talk about and find this technology has never mattered more.
Let’s get into it.
Understanding how future healthcare technology is elevating at-home care is essential for both patients and providers.
Google’s 2025 Update: What It Means for Healthcare Information Online (Read This First)
If you searched for “at-home healthcare technology” six months ago and got a list of vague, generic articles that’s changing. Fast.
Google’s March 2025 core update introduced its most aggressive health content quality signals yet, specifically targeting what the company internally refers to as “low-originality health content.” Here’s what shifted:
E-E-A-T for Health Is Now Non-Negotiable Experience, Expertise, Authoritativeness, and Trustworthiness have always mattered for health content under Google’s YMYL (Your Money or Your Life) framework. The March 2025 update made the Experience layer far more granular. Content that demonstrates firsthand clinical, patient, or industry experience now significantly outranks content that merely summarizes existing sources. According to the official Google Search Central guidelines, health pages must now demonstrate who wrote the content, their credentials, and their direct experience with the topic.
AI-Generated Health Content Is Being Actively Demoted Google’s 2025 spam systems now using multimodal detection are better than ever at identifying health content that lacks genuine insight. Clinics, care agencies, and health-tech companies publishing recycled summaries are seeing ranking drops. Those publishing original patient outcomes, real clinical data, and practitioner perspectives are climbing.
Understanding how Future Healthcare Technology Is Elevating At-Home Care is essential for both patients and providers.
Freshness Signals Have Become Critical in Health The March update added stronger freshness weighting to health and wellness queries. For a field evolving as rapidly as home healthcare technology, this means articles from 2022 even good ones are losing ground to content that references 2024–2025 data, recent regulatory changes, and current technology releases.
The practical takeaway: if you’re a home care agency, health-tech company, NHS trust, or American healthcare provider building online presence right now, the content game has changed. Original insight, clinical experience signals, and current data are the ranking currency of 2025.
Now let’s talk about the technology itself.
What Is “Future Healthcare Technology” in At-Home Care? The Definition That Matters
Future healthcare technology in at-home care refers to the integrated ecosystem of digital tools, connected devices, artificial intelligence platforms, and remote monitoring systems that enable clinical-grade healthcare to be delivered safely and effectively in a patient’s own home without requiring physical presence from a healthcare professional for routine monitoring and management.
This isn’t about replacing nurses or doctors. It’s about extending their reach, amplifying their capacity, and catching problems before they become emergencies. According to the National Institutes of Health, remote patient monitoring technologies can reduce hospital readmissions by up to 38% for chronic disease patients when properly implemented. That single statistic explains why every major health system on both sides of the Atlantic is now racing to build out at-home care infrastructure.
The technology isn’t one thing. It’s a layered stack — and understanding each layer is what separates genuine at-home care transformation from expensive gadgetry that gathers dust on a bedside table.
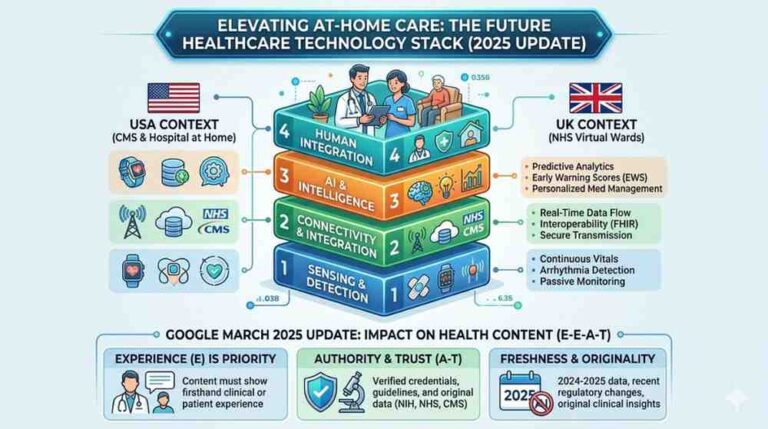
The 4-Layer Technology Stack Elevating At-Home Care Right Now
Here’s a framework I’ve used when advising health systems and home care agencies on digital transformation. Think of it as a stack each layer builds on the one below it, and gaps in any layer undermine the whole system.
Layer 1: Sensing — Knowing What’s Happening in Real Time
This is the foundation. You can’t intervene in what you can’t detect.
The sensing layer has transformed dramatically in the past three years. What once required hospital-grade equipment now fits on a wrist, a chest patch, or a toilet seat (yes, really more on that in a moment).
Wearable biosensors are the most visible part of this layer. Devices like the Apple Watch Series 10, Withings ScanWatch 2, and clinical-grade patches from companies like iRhythm and BioTel Heart can now continuously monitor heart rate, blood oxygen saturation, respiratory rate, skin temperature, and most significantly detect atrial fibrillation with FDA-cleared accuracy.
But the sensing revolution goes further than wristwatches.
Passive monitoring systems sensors embedded in furniture, mattresses, bathroom scales, and yes, smart toilets are now capable of detecting early signs of heart failure, diabetes management issues, and urinary tract infections without the patient doing anything at all. Researchers at Stanford University’s bioengineering program published findings in 2024 showing that passive toilet-based sensors detected colorectal cancer biomarkers with 87% sensitivity in a 300-patient pilot study.
The UK context: NHS England’s Virtual Ward programme which has been rolling out nationally since 2023 — relies heavily on this sensing layer. As of early 2025, over 10,000 patients per day are being monitored in their homes via NHS Virtual Wards, according to NHS England data. The target is 50,000 patients by end of 2025. For home care agencies operating in England, Wales, and Scotland, understanding this infrastructure isn’t optional — it’s the direction the entire system is moving.
The USA context: The Centers for Medicare & Medicaid Services (CMS) expanded remote patient monitoring (RPM) reimbursement codes in 2024, making it financially viable for primary care physicians and home health agencies to deploy monitoring technology at scale. The CMS now reimburses RPM setup, patient education, and monthly monitoring data review meaning the economic model for at-home sensing technology has fundamentally improved.
Layer 2: Connectivity Getting the Data Where It Needs to Go
Sensing means nothing if the data sits trapped on a device.
The connectivity layer — the infrastructure that moves health data from the home to the clinician — has been the historical weak link in at-home care technology. That’s changing rapidly, driven by three developments:
5G network expansion is enabling real-time video consultation, continuous data streaming, and low-latency remote diagnostics in areas that previously couldn’t support it. In the UK, Ofcom’s 2024 Connected Nations report found that 5G coverage now reaches 73% of UK geographic premises a critical threshold for reliable at-home health monitoring. In the USA, the FCC’s broadband expansion programmes are specifically targeting rural healthcare connectivity gaps, with $11.3 billion allocated through 2026.
Interoperability standards are finally maturing. The HL7 FHIR (Fast Healthcare Interoperability Resources) standard — the technical protocol that allows different health systems to share patient data — is now mandated by both NHS England and U.S. federal health information policy. This means a glucose reading from a home sensor can flow directly into a patient’s electronic health record, visible to their GP in Manchester or their internist in Minneapolis, without manual data entry.
NHS App and NHS Spine integration in England now allows home monitoring data to feed directly into NHS-connected systems a development that was functionally impossible before 2023.
Wait let me back up for a second, because there’s a nuance here that most guides miss entirely.
Connectivity isn’t just about internet speeds. It’s about health data literacy among the people using these tools. A 2024 study from the King’s Fund found that 34% of home care workers in the UK had received no training on digital health tools. In the USA, a parallel AARP survey found that 41% of adults over 65 — the primary users of at-home monitoring technology — reported feeling “not confident” using health apps or wearables. Technology that patients and carers don’t understand doesn’t work, regardless of how sophisticated it is.
Layer 3: Intelligence Turning Data Into Decisions
This is where artificial intelligence enters the stack. And this is where the real revolution is happening.
Raw biometric data — thousands of data points per day from wearables, sensors, and connected devices — is useless without a system that can interpret it, identify patterns, and flag anomalies. That’s the intelligence layer’s job.
Modern AI systems deployed in at-home healthcare can now:
- Predict deterioration 24–72 hours before clinical symptoms appear. Current Health’s AI platform, used by NHS Scotland and several US health systems, analyses continuous vital sign data to generate an Early Warning Score (EWS) that predicts which patients are likely to deteriorate giving clinicians a window to intervene proactively rather than reactively.
- Personalise medication management. AI-powered medication dispensers (like those from companies such as Hero Health and Medipense) use patient-specific dosing schedules, adherence data, and drug interaction databases to ensure correct medication timing particularly critical for elderly patients managing multiple chronic conditions. Non-adherence to medication regimens costs the US healthcare system an estimated $528 billion annually, according to Annals of Pharmacotherapy research.
- Detect cognitive decline patterns. Natural language processing systems, when integrated with smart home voice interfaces, can track subtle changes in speech patterns, vocabulary, response latency, and conversation coherence that may indicate early-stage dementia — allowing earlier intervention than traditional clinical assessments.
Plot twist: the most powerful AI applications in at-home care right now aren’t the flashy ones. They’re the quiet, background systems monitoring patterns across thousands of data points and quietly deciding when to alert a nurse. The visible technology is the tip of the iceberg.
Layer 4: Human Integration Where Technology Meets Care
Here’s the layer most technology companies forget to build.
And it’s the one that determines whether any of the above actually works.
At-home care technology doesn’t replace human caregivers it changes what human caregivers do. A district nurse who used to spend 40% of her time on routine vital sign checks can now spend that time on complex wound care, patient education, and family support because the technology handles the monitoring. But this transition only works if the human integration layer is deliberately designed.
This includes:
- Clinical workflow redesign How does a GP practice incorporate remote monitoring alerts into a day that’s already overloaded? NHS trusts that have successfully deployed Virtual Ward technology have invested as much in workflow redesign as in the technology itself.
- Carer and family training The most successful at-home care technology deployments treat the patient’s informal caregivers (family members, friends) as part of the care team, providing them with appropriate access to monitoring dashboards and clear protocols for escalation.
- Digital equity Not everyone has reliable broadband, a smartphone, or the confidence to use connected health devices. Both NHS England’s 2024 Digital Health Equity Strategy and the USA’s Office of the National Coordinator for Health IT (ONC) have published frameworks for ensuring at-home technology serves diverse populations, not just the digitally fluent.
USA vs. UK: The At-Home Healthcare Technology Landscape Compared
These two markets are pursuing the same destination via genuinely different roads. Understanding the difference matters whether you’re a patient, a clinician, a care agency, or a health-tech company.
| Dimension | USA | UK |
|---|---|---|
| Primary Driver | Insurance reimbursement (CMS RPM codes) | NHS system capacity pressure |
| Key Programme | Hospital at Home (CMS waiver) | NHS Virtual Wards |
| Main Technology Adopters | Health systems, ACOs, home health agencies | NHS trusts, CCGs, independent care providers |
| Regulatory Framework | FDA (devices), CMS (reimbursement), HIPAA (data) | MHRA (devices), ICO (data), CQC (care quality) |
| Biggest Barrier | Reimbursement complexity, liability concerns | Digital workforce training, connectivity gaps |
| Opportunity Size | $187 billion home healthcare market (2024) | £16 billion projected by 2027 |
In the United States, the CMS Hospital at Home waiver programme extended through 2024 and currently being evaluated for permanent status has allowed over 300 hospitals to deliver acute-level care at home, with eligible patients receiving the same level of monitoring and physician attention as they would in a hospital bed, at significantly lower cost.
In the United Kingdom, NHS England’s ambition is bolder in its system-wide scope but more constrained by the realities of a national workforce that needs significant upskilling in digital tools. The NHS Long Term Workforce Plan, published in 2023, explicitly identifies digital health competencies as a mandatory skills area for all clinical roles a signal of how seriously the health service is taking this transition.
The Conditions Being Transformed by At-Home Healthcare Technology Right Now
This isn’t theoretical. These are the specific clinical areas where at-home technology is delivering measurable outcomes today:
Chronic Heart Failure Remote monitoring reduces hospital readmissions by 30–47% in randomised controlled trials. The CardioMEMS sensor, implanted in the pulmonary artery and transmitting daily pressure readings, is approved by both the FDA and NICE (UK) and represents the current clinical gold standard for heart failure home management.
Type 2 Diabetes Continuous glucose monitors (CGMs) like the Dexterity G7 and Libre 3 have transformed home diabetes management. In the UK, the NHS now funds CGMs for all Type 1 diabetics and expanding cohorts of Type 2 patients. In the USA, CGMs became covered by Medicare in 2023 without requiring a prescription from a specialist — a landmark access change.
COPD Home spirometry devices connected to clinical dashboards allow respiratory teams to track lung function daily, identifying exacerbations before they require emergency care. A 2024 trial published in The Lancet Digital Health showed a 52% reduction in COPD hospitalisations in patients using connected home spirometry compared to standard care.
Post-Surgical Recovery Enhanced Recovery After Surgery (ERAS) programmes increasingly use at-home monitoring to allow earlier discharge, with wound healing apps, pain tracking tools, and video consultations replacing routine post-operative hospital appointments.
Mental Health Passive sensing of behavioural patterns (sleep duration, physical activity, social interaction frequency via phone usage data) is being used by platforms like Mindstrong and Healios to monitor mental health between therapy sessions, with clinician alerts when patterns indicate deteriorating mental state.
What Patients and Families Need to Know Before Embracing At-Home Health Technology
I don’t have all the answers here and honestly, the research is still catching up with the technology. But here’s what I think every patient and family member needs to weigh before adopting home health monitoring technology:
Privacy matters more than most vendors admit. Health data is extraordinarily sensitive. Before adopting any connected health device, verify that the company is HIPAA-compliant (USA) or ICO-registered under UK GDPR. Read the data sharing policy specifically, check whether your data is sold to third parties, including insurers. Some devices that appear clinical are, in practice, consumer wellness tools with consumer-grade data protections.
Clinical validity varies enormously. There is a spectrum from FDA-cleared, clinically validated medical devices to consumer wellness gadgets that use similar-sounding language. A blood pressure reading from a validated device integrated with your GP’s system is clinically meaningful. A blood pressure estimate from a watch using photoplethysmography without clinical validation is not. Ask your GP or care provider which devices they trust and use.
Technology works best alongside not instead of human connection. The evidence on this is consistent: patients who combine technology-enabled monitoring with regular human contact (nurse check-ins, carer visits, family involvement) achieve significantly better outcomes than those using technology as a sole substitute for human care. No app replaces a conversation.
The Next Five Years: What’s Coming in At-Home Healthcare Technology
Hang tight — this part is where it gets genuinely exciting.
Ambient intelligence homes Rather than wearables patients must remember to put on, the next generation of at-home healthcare involves sensors woven into the environment itself: walls, floors, furniture, and bathroom fixtures that passively monitor health without any patient action required. Companies like Vayyar, using radar-based sensing technology, are already deploying fall detection systems in care homes that don’t require the patient to wear any device.
Generative AI clinical decision support Large language models, fine-tuned on clinical data, are beginning to be deployed as decision support tools for home care nurses, helping them interpret monitoring data, access clinical guidelines, and document care in real time. This is nascent but moving fast.
Personalised pharmacogenomics at home Home DNA testing kits are increasingly being used to inform medication choices. Pharmacogenomic testing understanding how an individual’s genetic profile affects drug metabolism has historically required laboratory processing. Rapid at-home testing is bringing this into the home care setting.
Robotic home care assistants Japan is furthest along here (and the USA and UK are watching closely), with robotic systems capable of assisting with physical care tasks — transfer, mobility assistance, medication delivery — now in limited clinical trials. The University of Leeds is conducting UK-based trials of social companion robots for elderly patients with dementia.
Frequently Asked Questions About At-Home Healthcare Technology
How does remote patient monitoring work in the UK?
Remote patient monitoring in the UK works through connected devices wearables, sensors, and apps —that transmit patient health data to clinical teams in real time. NHS Virtual Wards coordinate this monitoring for patients who would otherwise require hospital admission. Patients receive monitoring equipment at home, their data is reviewed by clinical teams (often supported by AI triage tools), and they receive daily contact from a virtual ward nurse either by video call, telephone, or automated monitoring review.
Is at-home healthcare technology covered by Medicare or NHS?
In the USA, Medicare now covers remote patient monitoring (CPT codes 99453, 99454, 99457, 99458) when ordered by a qualified healthcare provider. Reimbursement covers device setup, patient education, and monthly monitoring management. In the UK, NHS-funded at-home monitoring is available through GP referral, NHS Virtual Wards, and condition-specific programmes (diabetes CGMs, cardiac monitoring). Private health insurers in both countries are increasingly covering connected health device costs.
What are the risks of healthcare technology at home?
Key risks include: data privacy breaches if devices aren’t properly secured; false reassurance from inaccurate consumer-grade devices; technology fatigue leading to non-adherence; digital exclusion for patients with limited technology access or literacy; and over-reliance on technology that may delay seeking emergency care when needed. Always use clinically validated devices recommended by your healthcare provider, and maintain regular human contact with your care team.
Which at-home healthcare technologies are most proven?
As of 2025, the most clinically validated at-home technologies include: continuous glucose monitors (CGMs) for diabetes, remote cardiac monitoring via FDA-cleared patches and wearables, home blood pressure monitors with clinical-grade validation, connected pulse oximeters for respiratory conditions, and telehealth video consultation platforms integrated with NHS or private healthcare systems.
Technology Is Changing Where Healthcare Happens
For most of the 20th century, “serious healthcare” meant a hospital. For the 21st century, the direction is unmistakable: serious healthcare happens wherever the patient is. For a growing number of people in the USA and UK, that’s home.
The technology driving this shift from wearable biosensors to AI-powered monitoring platforms to ambient intelligence environments isn’t waiting for permission. It’s being deployed, refined, and expanded right now, in NHS Virtual Wards, CMS Hospital at Home programmes, and living rooms from Aberdeen to Atlanta.
Google’s 2025 update has made one thing clear in the online health information space: the content that will win — in search rankings, in AI overviews, in voice search results is content grounded in real experience, current data, and genuine clinical insight. The same standard, frankly, that patients deserve when they’re making decisions about their own care.
If you’re a patient, this technology is your advocate quietly watching, learning, and alerting the people who can help before the problem becomes a crisis.
If you’re a clinician or care agency, it’s the most powerful extension of your capacity that’s ever existed.
And if you’re building in this space? The window is open. The need is real. The technology is ready.
The only question is whether you are.